July 27, 2020
Cancer and loneliness: How inclusion could save lives

COVID-19 has ignited a worldwide conversation about inequality. The question is whether we just want to talk about inequity or make the changes to produce more fair outcomes.
Focusing our efforts on one critical change would reduce disparities in some of the most pressing health issues of our time. That change is pluralism, the active process of inclusion: recognizing, valuing and respecting differences.
We can recognize ethnic variability in cancer treatments by diversifying clinical trial recruitment and improve deadly loneliness by including patients in treatment design.
Patients do better when differences are embraced rather than avoided. Health and research organizations must not be tourists, but participate actively in the full richness of their communities.

Racialized groups disproportionately bear the burden of loneliness, including the most severe catagory: desolate
Pixabay
As a physician and director in our medical school’s Office of Indigenous, Local and Global Health, I see in my patients the health consequences of exclusionary policies and practices. Pluralism could improve their lives and reduce illness from two very different conditions: cancer and loneliness.
Cancer
“Pharmacoethnicity” describes ethnic diversity in drug response or toxicity. Two people of different ethnicities might respond differently to the same cancer treatment dose, based on their environment and genetics.
People of European ancestry account for 81 per cent of registered genomes according to a paper in Nature. Drug makers use genomes to look for unique disease variations. So many of the groups with worse cancer outcomes, including Black, Indigenous and people of colour (BIPOC), may have unique disease variations but are excluded from the process of drug development. And once drugs are in testing, clinical trials for cancer medications continue to be characterized by an overrepresentation of white and male participants, at 80 per cent and 59.8 per cent, respectively.

Black and Hispanic patients are as willing to participate in clinical trials as white patients
Shutterstock
In the United States, of the thousands of patients in cancer clinical trials that led to 17 new drug approvals in 2018, only four per cent were Black or African American and four per cent were Hispanic, despite national populations of 13 per cent and 18 per cent respectively, according to the U.S. Food and Drug Administration. Indigenous Peoples are also underrepresented in clinical trials.
This under-representation is not for lack of interest; it is due to shortcomings in the recruitment process. In fact, Black and Hispanic patients are as willing to participate in biomedical research as white patients.
We cannot pretend that patients of all backgrounds respond the same to drug therapies when their environment and genetics are different. There are known examples among East Asians who experience high levels of toxicity when being treated for head and neck cancers. These patients can be treated effectively at a lower dose. In a lung cancer study that had a mix of Asian and white patients, a high side-effect rate in Asians led to a mid-trial dose reduction in Asian patients. But despite the dose reduction, Asians experienced a more impressive tumour response than whites. Ethnicity in clinical trials matters.
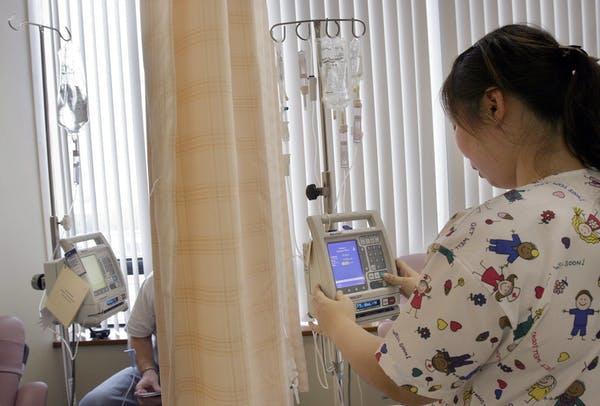
A nurse prepares a patient’s chemotherapy medication. Pharmacoethnicity describes ethnic diversity in drug response or toxicity
AP Photo/Wong Maye-E
We can increase diversity of enrolment in clinical trials through policies and practices of inclusion. Enrolment of Black patients rose by 62 per cent over two years after the introduction of a new program that emphasized presence in community and cultural competence. This approach embedded cancer prevention and research activities in the community. Simply being present and culturally aware dramatically improved recruitment, moving beyond mere statements about inclusion towards actionable value of diversity.
Similarly, in the U.S., Indigenous populations state a need for culturally competent partnerships with Indigenous communities. In order to improve health outcomes, scientists and scientific organizations need to be present in BIPOC communities and learn to understand and communicate across cultures; BIPOC communities are willing.
Loneliness

Loneliness is associated with a 26 per cent increased risk of premature death
Pixabay
We also ignore lonely and isolated people — and they are dying from this exclusion. Sounds dramatic, but this is borne out by evidence. Loneliness is associated with a 26 per cent increased risk of premature death, and a greater risk of heart disease and stroke. And loneliness is incredibly widespread: it affects one-third of people in the industrialized world. Again, racialized groups disproportionately bear the burden of loneliness. Racialized and Indigenous Canadians are also more likely to fall into the most severe category of loneliness: desolate. Elder minorities in Great Britain experience loneliness levels up to five times higher than the general population.
Loneliness can be diagnosed quickly using an easy three-question survey, but there is no prescription, medical device or surgical treatment. Successful treatment programs are customized to the patient and engage the intended participants in the design. These interventions are successful because they acquire nuanced understanding of the characteristics, cultures and perspectives of patients and communities.
Pluralism
Inclusion is not a checkbox. Pluralism requires us to change organizational structures to participate in communities.
Cancer treatment and research programmes must ensure BIPOC communities are consulted and included in trials to ensure equitable access to appropriate care. However, as with loneliness, inclusive treatment design does not only benefit BIPOC communities but any lonely patient, each with their own rich personal history.
Academic and health leaders must hold themselves and their organizations accountable by enshrining policies that recognize, value and respect difference. As private citizens, we must hold our elected officials, educators, clinicians and scientific institutions to account.
It is time to move beyond checkbox-inclusion and towards building and sustaining nuanced relationships with communities.
COVID-19 has changed our ways of living. We have been forced to adapt to a new virus. Let’s keep changing, and replace exclusive old traditions with a new era of inclusive medicine.



