Dec. 9, 2013
Boosting the immune system to treat brain cancer

V. Wee Yong, PhD, and research associate Susobhan Sarkar, PhD.
Researchers at the University of Calgary’s Hotchkiss Brain Institute (HBI) have made a discovery that could lead to better treatment for patients suffering from brain cancer.
Despite current treatment strategies, the median survival for patients with the most aggressive brain cancer – called glioblastoma, is 15 months. Less than five per cent of patients survive beyond five years.
Our brain’s natural defense, compromised
HBI member V. Wee Yong, PhD and research associate Susobhan Sarkar, PhD, and their team including researchers from the Department of Clinical Neurosciences and the university’s Southern Alberta Cancer Research Institute, looked at human brain tumour samples and discovered that specialized immune cells in brain tumour patients are compromised. The researchers took this discovery and, in an animal model, identified a drug that is able to re-activate those immune cells and reduce brain tumour growth, thereby increasing the lifespan of mice two to three times. Their discovery was published December 8 in the prestigious journal Nature Neuroscience.
Our brains normally contain specialized cells, called microglia, that defend against injury or infection. “Microglia are the brain’s own dedicated immune system,” explains Yong. “And in this study, we have formally demonstrated for the first time that these cells are compromised in living brain tumour patients.”
As with other forms of cancer, brain tumours start as individual stem-like cells – called brain tumour initiating cells (BTICs). These cells quickly divide and grow, eventually forming a mass, or tumour. Yong and his team have discovered that the tumour disables microglia, permitting the rapid proliferation of BTICs, which ultimately leads to brain tumour growth.
“We refer to this as the battle for the brain, in which early on in the disease, the microglia are trying to destroy the brain tumour initiating cells,” says Yong. “But over the course of time, the tumour disables the microglia and we start to see more initiating cells and more rapid tumour growth. We have sought to tip the battle in favour of the brain to suppress the tumour.”
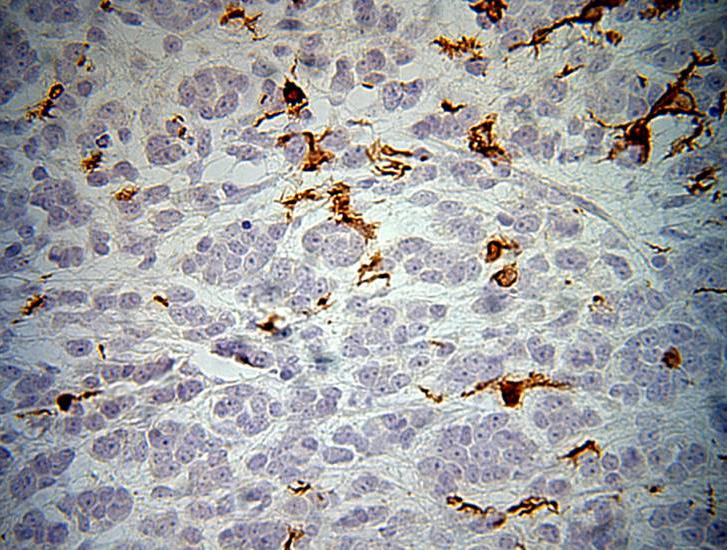
Brain of control subject.
Therapeutic re-activation of immune cells
In addition to discovering this mechanism, Yong and Sarkar also identified a drug - amphotericin B (AmpB) - to reactivate microglia that in an animal model, showed a significant reduction in brain tumour growth.
“This drug was able to re-activate the disabled microglia,” says Sarkar, “thus restoring the body’s natural defense mechanisms and restricting the growth of brain tumour initiating cells.”
The drug they identified is a powerful agent that is already used clinically to treat severe fungal infections of the brain and spinal cord. “It’s a rather harsh medication,” says Yong. “But we have demonstrated that this drug can be used in very small doses where it is not only well tolerated, but it is also effective in re-programming microglia.”
Yong and Sarkar hope this discovery will lead to clinical trials and ultimately to a new standard of care for brain tumour patients.
A new approach to treating brain cancer
“This opens up an entirely new field of research with tremendous clinical potential,” says Yong. “Our hope is that clinicians will pick up this idea and use our findings in a clinical trial.”
The standard treatment right now for brain tumour patients is usually a combination of surgery, chemotherapy and radiation. “All of these treatments currently focus on reducing tumour growth,” says Sarkar. “But if we can use those treatments in combination with a method of enhancing the brain’s immune system, we would have a two-pronged approach that has tremendous therapeutic potential.”
As Yong puts it, “our research suggests adding another tool to the toolbox to fight this devastating disease. If we can boost the immune system and allow microglia to do their job and control brain tumour stem cells, it would be like removing the seed from the soil – stopping the tumour growth before it starts to get out of control.”
The finding has already garnered attention from researchers across Canada, including internationally recognized brain tumour scientist and neurosurgeon Dr. James Rutka, Professor and Chair, Department of Surgery, University of Toronto and Dr. Rolando Del Maestro, William Feindel Professor Emeritus in Neuro-Oncology, McGill University.
“This research is highly significant as it implies that a commercially available drug, amphotericin B, which has never been used before for patients with gliomas, may be a novel treatment to consider in future trials of patients with this frequently lethal cancer,” says Dr. Rutka.
Dr. Del Maestro adds, "Yong and colleagues at the University of Calgary have begun to unravel the complex interaction of the microglia with the brain tumor cells, resulting not only in furthering our understanding, but providing a new concept and drug which can now be immediately assessed in clinical trials."
Funding was provided by Alberta Innovates – Health Solutions/Alberta Cancer Foundation. V. Wee Yong is a Canada Research Chair in Neuroimmunology.
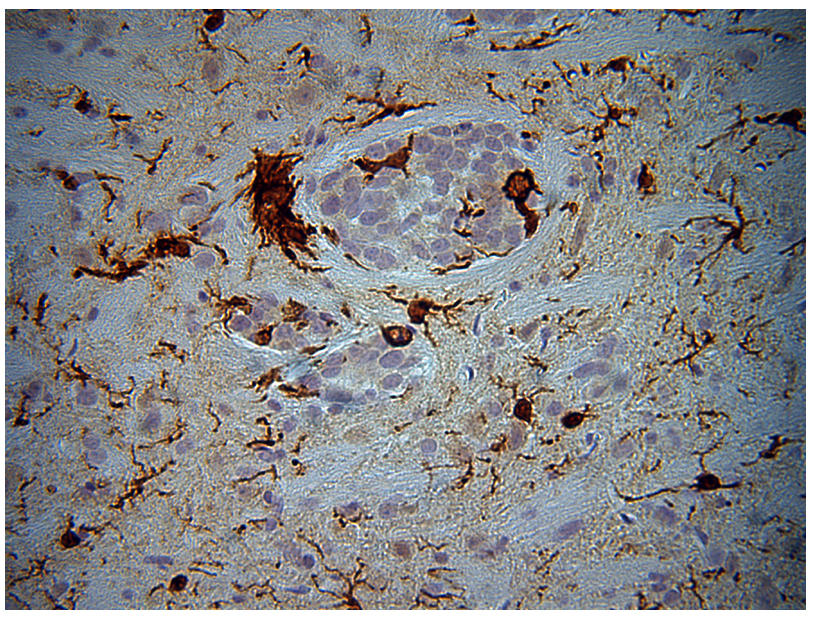
Brain of treated experimental subject.
